
In theory, WCB is designed to support workers who experience injuries or illnesses as a result of their work. For physical injuries, the process is relatively straightforward. However, for psychological injuries—such as PTSD, anxiety, or burnout—the process is anything but easy.
The Checklist of Frustration
To report a psychological injury, nurses must first navigate a complex maze of forms and checklists. These often require detailed information that may be difficult for the worker to provide, especially when dealing with the emotional impact of trauma. This can lead to incomplete or inaccurate submissions, delaying the process or even resulting in a denied claim.
Once a report is submitted, the nurse is typically subjected to a series of investigations. However, WCB claims agents are often not trained to handle the nuances of psychological injuries, particularly those caused by high-stress professions like nursing. For many, the investigation process can feel like an additional layer of stress and confusion, undermining their mental health instead of supporting their recovery.
Re-traumatization Through Repetition
Perhaps the most damaging aspect of the WCB process is the repeated need for nurses to recount their traumatic experiences. Nurses may be asked to tell their story multiple times to different agents, write detailed reports, and attend multiple appointments. Each retelling can trigger a re-experience of the trauma, making it harder for the nurse to heal. For someone already struggling with PTSD, anxiety, or burnout, this repetition can make it feel like the system is less about recovery and more about punishment.
This repeated retraumatization often discourages nurses from continuing with their claims, leading them to abandon the process altogether or return to work before they are ready. The system intended to help them can often feel like an additional burden.
Nurses on the Frontlines of Crisis
Whether it’s responding to an emergency in the ER, providing life-saving care in ICU, or comforting a family as a loved one passes away, nurses are exposed to some of the most emotionally taxing experiences imaginable. Nurses also face increased risks of physical harm, including violence from patients in crisis or exposure to contagious diseases. Despite this, many nurses are expected to carry on without adequate support for their mental health.
As frontline workers, nurses are at an increased risk of psychological injury. Yet, when these injuries occur, the system often fails to recognize the trauma as a direct result of the nurse’s job. The solution? Presumptive legislation.
What is Presumptive Legislation?
Presumptive legislation automatically recognizes certain injuries—physical or psychological—as work-related, without requiring the worker to prove a direct causal link between the injury and their job. For nurses, this would mean that a psychological injury—whether PTSD, burnout, or anxiety—would automatically be assumed to have been caused by their work, without the need to recount traumatic events or prove the connection.
Presumptive coverage would streamline the process for nurses, making it easier for them to access compensation and focus on recovery instead of fighting bureaucratic barriers. It’s an essential step toward acknowledging the unique psychological risks that nurses face every day
Province Comparisons: Why Some Are Leading and Others Are Lagging
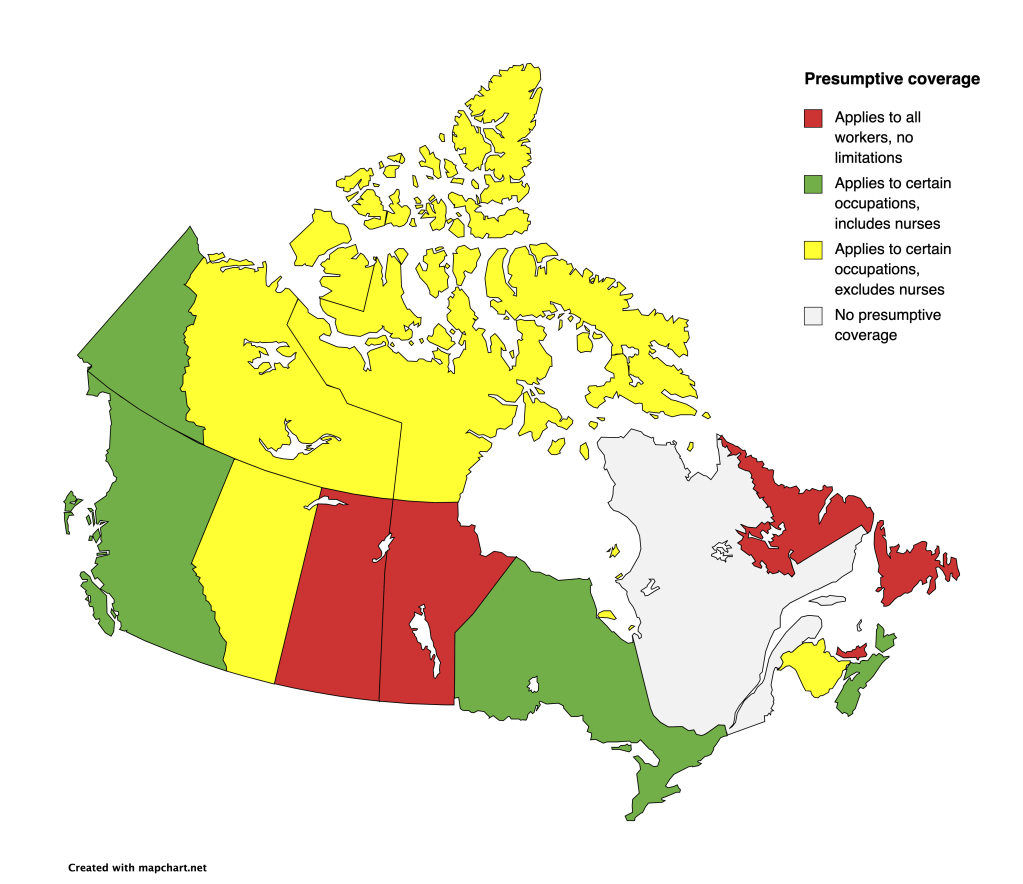
The disparity between provinces when it comes to presumptive legislation is significant. While some provinces have implemented policies that recognize the psychological toll of nursing, others—such as Alberta—have fallen behind, leaving nurses to navigate an unnecessarily complex and burdensome system.
Saskatchewan: Leading the Way
Saskatchewan is one of the most progressive provinces in Canada when it comes to supporting workers with psychological injuries. It was the first jurisdiction to implement presumptive legislation for all forms of psychological injury incurred through work, and this includes nurses. This means that if a nurse in Saskatchewan suffers from PTSD or any other psychological injury as a result of their work, they do not have to jump through hoops to prove that their trauma is work-related.
This approach eliminates the unnecessary and damaging process of recounting traumatic experiences and ensures that nurses can access the support they need quickly and easily.
Learn more about Saskatchewan’s policy here.
British Columbia: A Step Forward, But More Is Needed
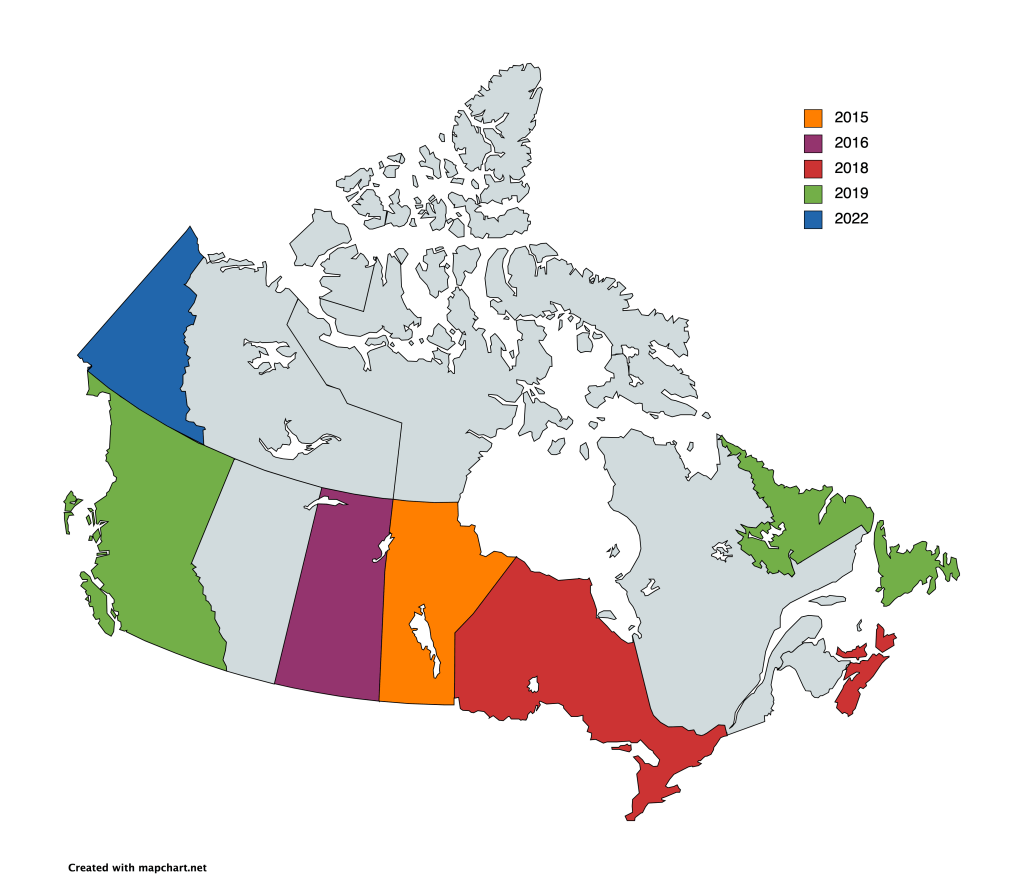
In 2019, British Columbia amended the Workers’ Compensation Act to include nurses in its presumptive legislation for psychological injuries. This change makes it easier for nurses to access compensation if they are diagnosed with a mental health condition related to their work. While this is a positive step, there are still gaps in the system, and many nurses continue to face barriers when seeking support. More work is needed to ensure that nurses in BC—and across the country—are fully supported.
Alberta: A Setback for Nurses
In Alberta, however, the situation is quite different. In 2018, the province made a significant change to the Workers’ Compensation Board (WCB) that excluded nurses from presumptive coverage for psychological injuries. While first responders like police officers, firefighters, and emergency medical services workers are covered under presumptive legislation, nurses are not.
This exclusion means that many nurses in Alberta who are suffering from PTSD, burnout, and other psychological injuries are left without the support they need. The ongoing burden of dealing with a complex claims process can prevent nurses from getting the care they need, potentially leading to further psychological harm.
Manitoba and Ontario: A Model for Change
Manitoba has had presumptive legislation for nurses since 2015, and Ontario followed suit in 2018. These provinces recognize that nurses are exposed to significant psychological risk in their work and that presumptive legislation is a vital step in supporting their mental health. By making it easier for nurses to access compensation, these provinces have taken a step toward ensuring that healthcare workers are cared for when they need it most.
Conclusion: Nurses Deserve Better
The current WCB process for nurses suffering from psychological injuries is broken. It is inefficient, burdensome, and ultimately retraumatizing. The repeated recounting of traumatic events, the need to navigate complex forms, and the absence of presumptive legislation leave nurses unsupported and vulnerable.
It’s time for a change. Nurses are on the frontlines of our healthcare system, and we must do more to support them. Presumptive legislation is essential for ensuring that nurses can access the care they need without further emotional strain.
Nurses work tirelessly to care for us—now it’s time for us to care for them. We must advocate for expanded presumptive legislation in all provinces, ensuring that nurses are supported when they experience psychological injuries as a result of their work.
Call to Action
If you’re a nurse, healthcare worker, or advocate for mental health in the workplace, now is the time to speak out. Advocate for expanded presumptive legislation in your province. Reach out to your local MLA and raise awareness about the flaws in the current WCB system. Ask your MLA to support a bill in the legislature to add nurses to presumptive legislation. Nurses deserve better. Let’s ensure that they receive the care and support they need to continue doing the vital work that keeps our healthcare system running.
Resources:
https://web2.gov.mb.ca/bills/40-4/b035e.php
https://www.wcb.ns.ca/Portals/wcb/PTSD%20Fact%20Sheet.pdf?ver=2018-10-17-105044-457

Leave a comment